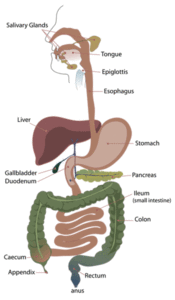
Stress. Most of us feel it with some regularity. We typically think in terms of difficult life circumstances – e.g., financial reversals, work-related challenges, loss of social standing, relationship issues, illness. But it can also accompany welcome life events – e.g., marriage, promotions, buying houses, retirement, vacations.
 I don’t like to admit to feeling stressed. I prefer to think that I have everything under control. That whatever life is throwing at me, I’ve got it covered. And I don’t like slowing down when I’ve got a full head of stream or taking things off my plate when I’m busy. Stress can be an unpleasant wake-up call that I’m not interested in answering.
I don’t like to admit to feeling stressed. I prefer to think that I have everything under control. That whatever life is throwing at me, I’ve got it covered. And I don’t like slowing down when I’ve got a full head of stream or taking things off my plate when I’m busy. Stress can be an unpleasant wake-up call that I’m not interested in answering.
Back in the 1960s, folks started taking an interest in the relationship between stress and illness. Psychiatrists Thomas Holmes and Richard Rahe examined the medical records of thousands of patients and correlated the incidence of illness with various life events. They published the following Holmes and Rahe Stress Scale through which the sum of change units in a given year provided an indication of the relative risk of illness. A score of 300+ suggested a high risk of illness, 150-299 moderate, and <150 slight.
| Life Event | Change Unit | Life Event | Change Unit |
| Death of a spouse | 100 | Child leaving home | 29 |
| Divorce | 73 | Trouble with in-laws | 29 |
| Marital separation | 65 | Outstanding personal achievement | 28 |
| Imprisonment | 63 | Spouse starts or stops work | 26 |
| Death of a close family member | 63 | Beginning or end of school | 26 |
| Personal injury or illness | 53 | Change in living conditions | 25 |
| Marriage | 50 | Revision of personal habits | 24 |
| Dismissal from work | 47 | Trouble with boss | 23 |
| Marital reconciliation | 45 | Change in working hours or conditions | 20 |
| Retirement | 45 | Change in residence | 20 |
| Change in health of family member | 44 | Change in schools | 20 |
| Pregnancy | 40 | Change in recreation | 19 |
| Sexual difficulties | 39 | Change in church activities | 19 |
| Gain a new family member | 39 | Change in social activities | 18 |
| Business readjustment | 39 | Minor mortgage or loan | 17 |
| Change in financial state | 38 | Change in sleeping habits | 16 |
| Death of a close friend | 37 | Change in number of family reunions | 15 |
| Change to different line of work | 36 | Change in eating habits | 15 |
| Change in frequency of arguments | 35 | Vacation | 13 |
| Major mortgage | 32 | Major holiday | 12 |
| Foreclosure of mortgage or loan | 30 | Minor violation of law | 11 |
| Change in responsibilities at work | 29 |
The system purportedly had value for folks like me who might ignore the signs of stress but rack up sufficient stressors to warrant a moment or two of consideration. Having run across this system recently, I got to thinking: Has their research stood the test of time?
An article by Cohen, Murphy, and Prather on stressful life events and disease risk provided several insights based on 70 years of research on the subject. Here are their findings:
- Stressful events may arise based on the amount of adaptation or change required of an individual, the imminence of threat or harm, a level of demand exceeding resources, an interruption of goals, or any combination thereof.
- Stressful events influence disease onset through a variety of mechanisms. As discussed in a prior post, excess stress may lead to hypertension, high cholesterol, disrupted digestion, bone disintegration, suppression of immune function, and neural network damage. The affected individuals may also adopt poor health behaviors as coping mechanisms – e.g., faulty nutrition, poor exercise habits, substance abuse, dysfunctional sleep patterns.
- Most people exposed to stressful events do not get sick. And despite increased risk for mental disorders, stress does not necessarily lead to depression. People with greater perceived control, self-efficacy, and a generally optimistic outlook tend to be resilient.
- Excluding natural disasters, stressful event exposure correlates with socioeconomic status (i.e., low status yields more events) and personality factors (e.g., agreeableness, conscientiousness, positive or negative attitude, attachment styles, neuroticism).
- Stressful events may not cause disease in otherwise healthy people. Nonetheless, biological wear and tear caused by chronic stress may result in increased disease risk, and stress may tip the balance toward disease in a system made vulnerable by other causes.
- Certain stressors are more impactful than others, notably those which threaten an individual’s sense of competence or standing in areas that reflect the individual’s core identity. These stressors generally fall within the domains of interpersonal problems, social status, and work difficulties. In particular:
- Stressful interpersonal events have been associated with heightened risk of depression, upper respiratory infection, hypertension, heart disease, physical disability, and premature mortality.
- Folks experiencing social rejection have shown decreased anti-inflammatory gene signaling and increased asthma symptoms.
- Unemployment and underemployment has been associated with increased risk of depression, cardiovascular disease, and premature mortality. Even a month’s worth of unemployed and underemployment increases susceptibility to cold-causing viruses.
- As a rule, persistent stress and chronic intermittent stress prove more deleterious than acute stress. Acute stress proves problematic when it accelerates a pre-existing disease process or sets off longer-term trauma (e.g., rape).
- Multiple events may or may not be more potent than individual ones. Studies have not done a good job accounting for multiple distinct stressors versus several events tied to a single root cause (e.g., divorce and associated changes in financial status, residence, church, social circles, recreation, etc.)
- The impact of stressful events varies as a function of when they occur during a life. For example, the death of a spouse at middle age with teenaged children proves more impactful than in one’s senior years. Moreover, there are sensitive periods in life when stressors exact a higher toll, notably childhood.
- Men and women respond to stress differently based on evolutionary pressures and cultural norms.